We’ve helped change the standard of care for people with diabetes, with open source automated insulin delivery.
–
I get citation alerts sometimes when my previous research papers or articles are cited. For the last few years, I get notifications when new consensus guidelines or research comes out that reference or include mention of open source automated insulin delivery (AID). At this time of year, the ADA Standards of Care is released for the following year, and I find out usually via these citation alerts.
Why?
This year, in 2023, there’s a section on open source automated insulin delivery!
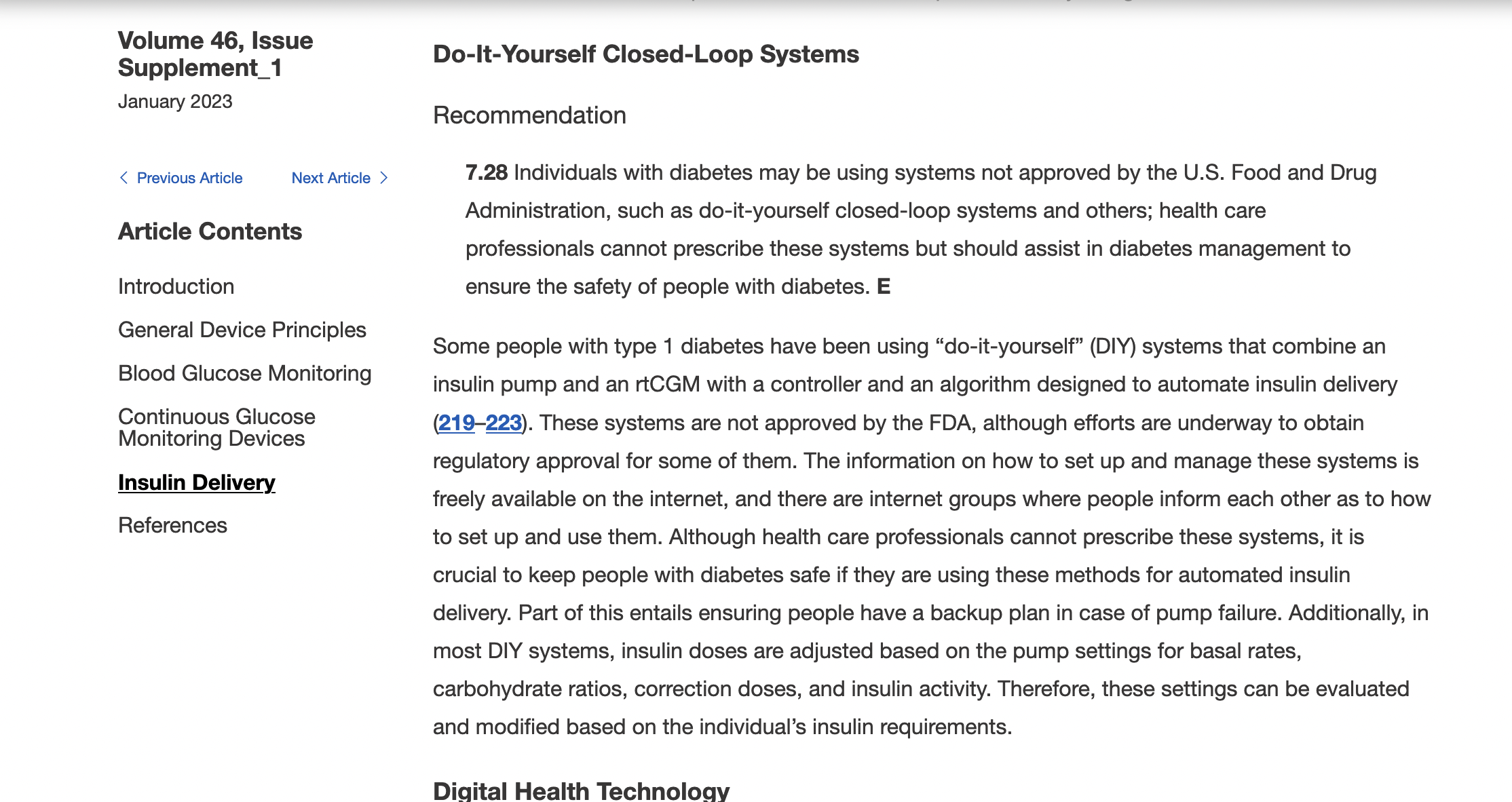
But did you know, that’s not really new? Here’s what the 2022 version said:
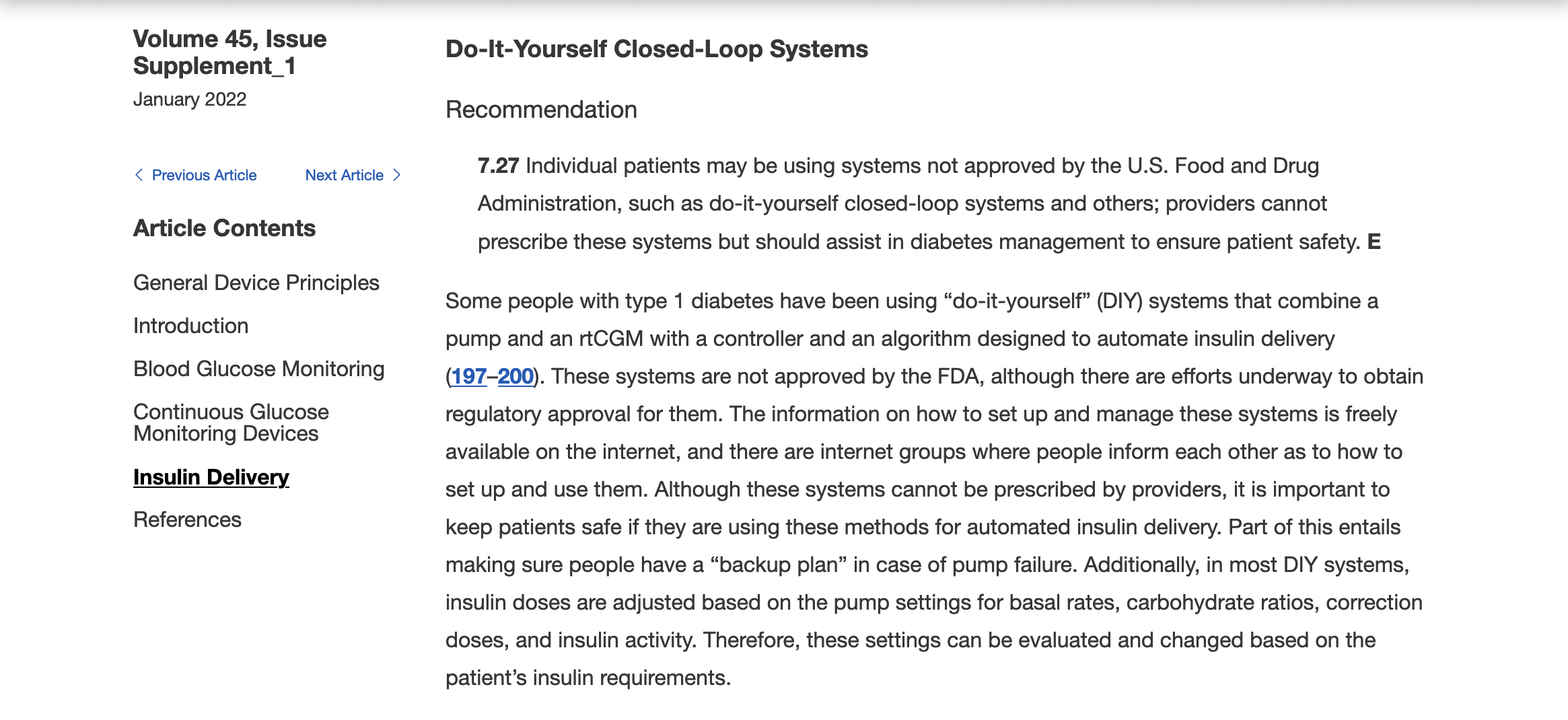
And 2021 also included…
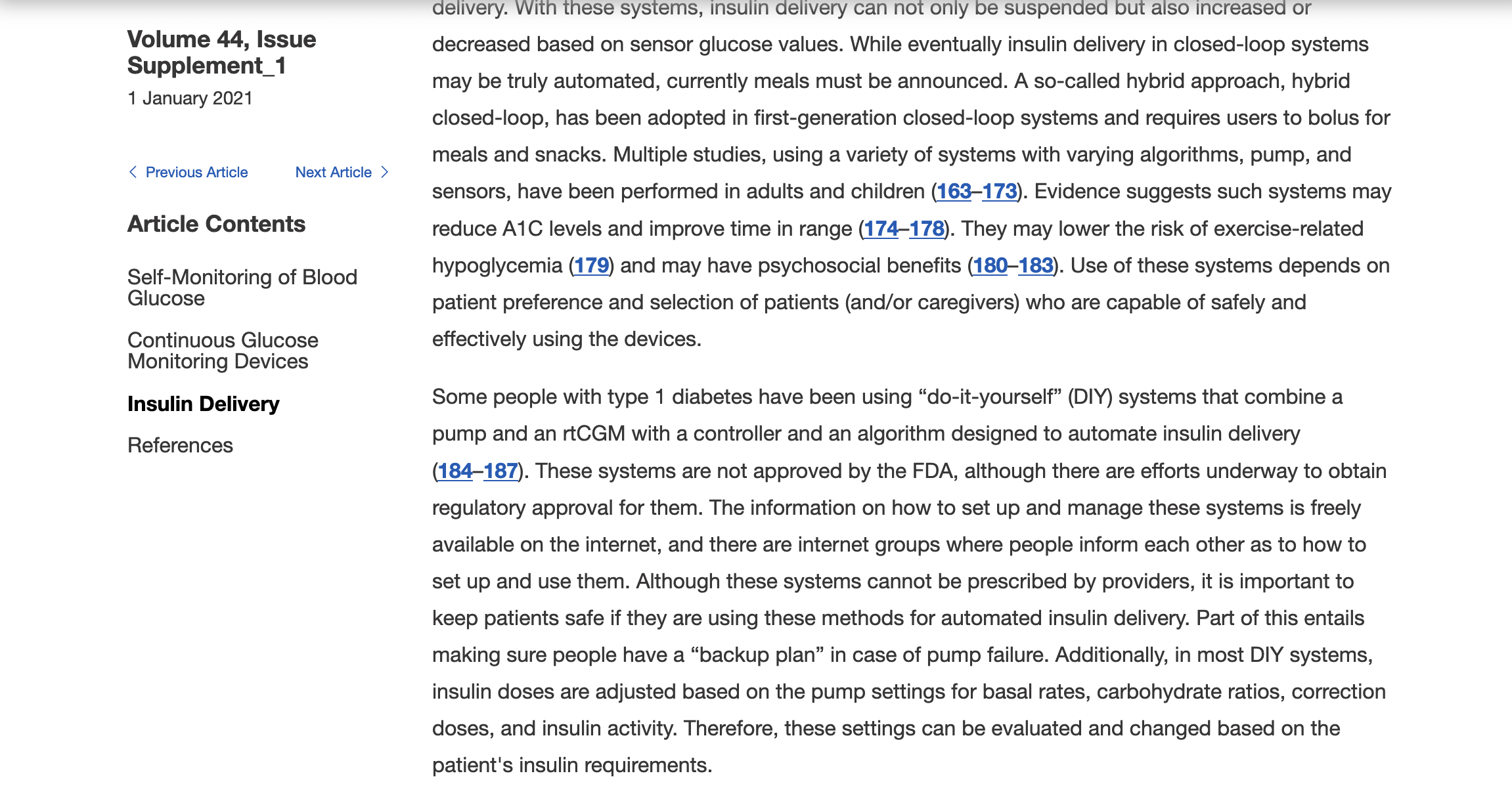
And 2020? Yup, it was there, too.

All the way back to 2019!
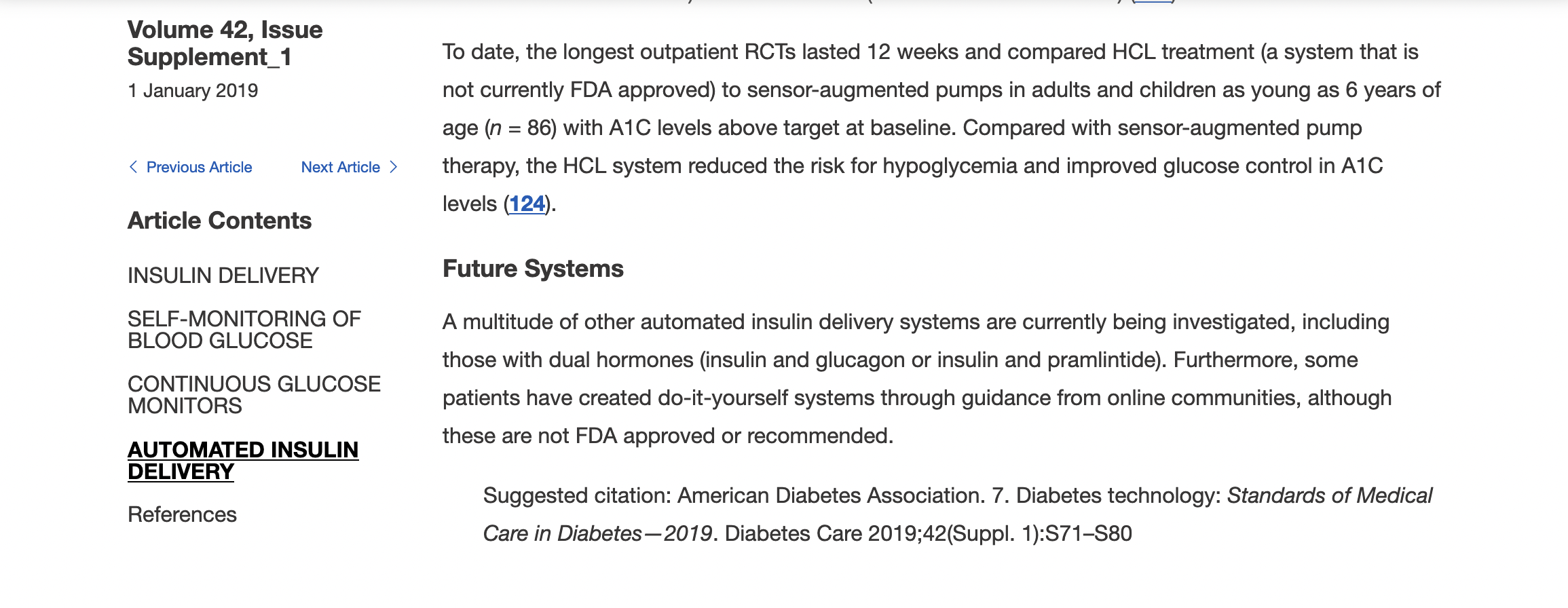

If you read them in chronological order, you can see quite a shift.
In 2019, it was a single sentence noting their existence under a sub-heading of “Future Systems” under AID. In 2020, the content graduated to a full paragraph at the end of the AID section (that year just called “sensor-augmented pumps”). In 2021, it was the same paragraph under the AID section heading. 2022 was the year it graduated to having its own heading calling it out, with a specific evidence based recommendation! 2023 is basically the same as 2022.
So what does it say?
It points out patients are using open source AID (which they highlight as do-it-yourself closed loop systems). It sort of incorrectly suggests healthcare professionals can’t prescribe these systems (they can, actually – providers can prescribe all kinds of things that are off-label – there’s just not much point of a “prescription” unless it’s needed for a person’s elementary school (or similar) who has a policy to only support “prescribed” devices).
And then, most importantly, it points out that regardless, healthcare providers should assist in diabetes management and support patient choice to ensure the safety of people with diabetes. YAY!
“…it is crucial to keep people with diabetes safe if they are using these methods for automated insulin delivery. Part of this entails ensuring people have a backup plan in case of pump failure. Additionally, in most DIY systems, insulin doses are adjusted based on the pump settings for basal rates, carbohydrate ratios, correction doses, and insulin activity. Therefore, these settings can be evaluated and modified based on the individual’s insulin requirements.”
You’ll notice they call out having a backup plan in case of pump failure.
Well, yeah.
That should be true of *any* AID system or standalone insulin pump. This highlights that the needs of people using open source AID in terms of healthcare support are not that different from people choosing other types of diabetes therapies and technologies.
It is really meaningful that they are specifically calling out supporting people living with diabetes. Regardless of technology choices, people with diabetes should be supported by their healthcare providers. Full stop. This is highlighted and increasingly emphasized, thanks to the movement of individuals using open source automated insulin delivery. But the benefits of this is not limited to those of us using open source automated insulin delivery; this spills over and expands to people using different types of BG meters, CGM, insulin pumps, insulin pens, syringes, etc.
No matter their choice of tools or technologies, people with diabetes SHOULD be supported in THEIR choices. Not choices limited by healthcare providers, who might only suggest specific tools that they (healthcare providers) have been trained on or are familiar with – but the choices of the patient.
In future years, I expect the ADA Standard of Care for 2024 and beyond to evolve, in respect to the section on open source automated insulin delivery.
The evidence grading should increase from “E” (which stands for “Expert consensus or clinical experience”), because there is now a full randomized control trial in the New England Journal of Medicine on open source automated insulin delivery, in addition to the continuation results (24 weeks following the RCT; 48 full weeks of data) accepted for publication (presented at EASD 2022), and a myriad of other studies ranging from retrospective to prospective trials. The evidence is out there, so I expect that this evidence grading and the text of the recommendation text will evolve accordingly to catch up to the evidence that exists. (The standards of care are based on literature available up to the middle of the previous year; much of the things I’ve cited above came out in later 2022, so it matches the methodology to not be included until the following year; these newest articles should be scooped up by searches up to July 2023 for the 2024 edition.)
–
In the meantime, I wish more people with diabetes were aware of the Standards of Care and could use them in discussion with providers who may not be as happy with their choices. (That’s part of the reason I wrote this post!)
I also wish we patients didn’t have to be aware of this and don’t have to argue our cases for support of our choices from healthcare providers.
But hopefully over time, this paradigm of supporting patient choice will continue to grow in the culture of healthcare providers and truly become the standard of care for everyone, without any personal advocacy required.
—
Note added in December 2024 – the 2025 Standards of Care now have evidence grade “B” and include the specific recommendation to “Support and provide diabetes management advice to people with diabetes who choose to use an open-source closed-loop system.”
You can find the 2025 Standard of Care section here.
